For Physicians
Clinically Validated, FDA Cleared
Meno√Check® is a unique blood test specifically designed to detect ultra-low levels of Anti-Mullerian Hormone (AMH) in serum. It is manufactured by Ansh Labs LLC and is FDA Cleared for measuring AMH in the determination of menopausal status.
MenoCheck is the only commercially available AMH immunoassay that has the sensitivity to detect ultra-low levels of AMH in menopausal women. The data supporting the use of the MenoCheck test was acquired from over 1500 women participating in a 20-year study, involving careful clinical observations and hormone measurements annually, as they underwent the menopausal transition and 12 months of amenorrhea to allow an accurate FMP date.
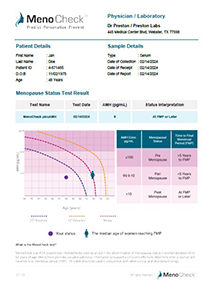
AMH Values and Time to Final Menstrual Period
The FMP for each woman in the SWAN Study were assigned retrospectively after 12 months of amenorrhea (the clinical definition of natural menopause). Menopausal categories for assigning status were based on the approximate time to the FMP. Three menopausal categories were defined based on the time to final menstrual period (TTFMP).
| Category | Menopausal Category | MenoCheck (pg/mL) |
| High | > 5 years from FMP | ≥100 pg/mL |
| Medium | < 5 years from FMP | 10-99.9 pg/mL |
| Low | at FMP or later | ≤10 pg/mL |
NOTE: AMH values are not commutable between brands. And, AMH results should always be assessed in conjunction with the patient’s medical history, clinical examination and other findings when being interpreted for diagnostic purposes.
Clinical Studies
The Study of Women’s Health Across the Nation (SWAN) was a multi-site longitudinal, epidemiologic study designed to examine the health of women during their middle years. This massive study resulted in 498 publications and countless scientific sessions and abstracts at medical conferences. Following are a select few that are specific to the menopausal transition.
Prediction of trans-menopausal bone loss using MenoCheck (picoAMH)
Objective
To predict the rate of bone loss over the trans-menopause using the serum levels of AMH in women early in the menopausal transition.
Methods
Serum samples from 3302 women aged 42 to 52 years were collected and picoAMH levels were measured. Bone Marrow Density in the lumbar spine and femoral neck was measured annually. The ability of AMH level to predict the annualized rate of BMD decline between the two visits (% decline per year) were tested.
Results
AMH inter-quartile range was [11,146] pg/mL. Median rate of BMD decline was 1.3% per year in the spine and 1.0% per year in the femoral neck. Adjusted for age, BMI, smoking, race/ethnicity, and study site, in multivariable linear regression, each 75% (or four-fold) decrement in AMH level was associated with 0.15% per year faster decline in spine BMD (p<0.001) and 0.13% per year faster decline in femoral neck BMD (p=0.005).
Conclusion
These findings suggest that serum levels of AMH in women going through the MT can indeed predict the rate of trans-menopausal bone loss, and help identify the women at risk of most loss. AMH levels appear to provide information about the rate of bone loss beyond that provided by serum levels of estradiol and FSH.
Reference:
Crawford S, Finkelstein J, Gold E, Greendale G, Harlow S, Joffe H, Kalra B, Kumar A, Martin D, Merillat S, Morrison A, Sluss P, Thurston R, Avis N. Predicting Onset of Menopausal Vasomotor Symptoms with Anti-Mullerian Hormone in the Study of Women’s Health Across the Nation (SWAN) Presented at 98th Annual Endocrine Society Meeting; 2016 Apr 1-3; Boston, MA
Associations of premenopausal AMH levels with lipids profile using MenoCheck (picoAMH)
Objective
To assess whether lower premenopausal AMH and greater declines in AMH levels over menopausal transition (MT) would be associated with adverse changes with lipid profiles.
Methods
Serum samples from 1423 women aged 42 to 52 years were collected and picoAMH and lipid including total cholesterol, triglycerides, high-density lipoprotein cholesterol (HDL-C), calculated low-density lipoprotein cholesterol (LDL-C), apolipoprotein A-1 (apoA-1), and apolipoprotein B (apoB) were measured.
Results
In unadjusted models, lower premenopausal AMH levels and greater declines in AMH over the MT were significantly associated with higher levels of lipids. [per 1 log unit decrease in premenopausal AMH: Cholesterol β(se): 2.76(0.38) , log Triglycerides: 0.01(0.01), LDL-C: 1.86(0.35), apoB: 1.45(0.31), HDL-C: 0.54(0.17), apoA-1: 0.83(0.30), P values <0.006; per 1 log unit decline in AMH over MT: Cholesterol β(se): 2.80(0.15) , log Triglycerides: 0.01(0.002), LDL-C: 2.12(0.13), apoB: 1.09(0.12), HDL-C: 0.46(0.05), apoA-1: 2.44(0.16), P values <0.0001]. These associations largely remained significant in final, multivariable models except for triglycerides
Conclusions
Women with less ovarian reserve as reflected by lower premenopausal AMH levels and greater declines in AMH over the MT had a worse lipid profile. Measuring AMH earlier in the MT could help identify premenopausal women at increased risk of later CVD.
Reference:
El Khoudary SR, Wang L, Brooks MM, Matthews KA, Thurston RC, Crawford S, Derby C, Jackson EA, Lee JS, Un-Yong Chae C, McConnell DS, Finkelstein J. Associations of Anti-Mullerian Hormone Premenopausal Levels and Their Changes over the Menopausal Transition with Lipids: The Study of Women′s Health Across the Nation (SWAN). Presented at 98th Annual Endocrine Society Meeting; 2016 Apr 1-3; Boston, MA
Predicting the onset of menopausal vasomotor symptoms with MenoCheck (picoAMH)
Objective
To assess whether AMH predicts the onset of frequent VMS symptoms and contributes to the information independent of other serum markers
Methods
Serum samples from 919 women (aged 42 to 52 years were collected and picoAMH, estradiol, FSH, were measured. VMS and menopausal status based on menstrual bleeding were measured annually.
Results
Of 919 participants, 297 had incident frequent VMS. AMH level was significantly negatively associated (p<.0001) with incident frequent VMS (HR 0.28, 95% CI 0.23 – 0.34). Similar statistical model fits for AMH, estradiol, FSH, and menopause status taken one at a time. Though, a slightly higher associations of VMS with FSH compared with the other three markers, AMH remained significantly associated (p<.001) with incident frequent VMS after adjusting for menopausal status (adjusted HR 0.29, 95% CI 0.22 – 0.39), for estradiol (adjusted HR 0.36, 95% CI 0.27 – 0.50), and for FSH (adjusted HR 0.55, 95% CI 0.42 – 0.71).
Conclusions
AMH is useful for predicting the incidence of VMS, particularly frequent VMS, independent of other key markers of menopause stage based on menstrual bleeding or other reproductive hormones.
Reference:
Crawford S, Finkelstein J, Gold E, Greendale G, Harlow S, Joffe H, Kalra B, Kumar A, Martin D, Merillat S, Morrison A, Sluss P, Thurston R, Avis N. Predicting Onset of Menopausal Vasomotor Symptoms with Anti-Mullerian Hormone in the Study of Women’s Health Across the Nation (SWAN) Presented at 98th Annual Endocrine Society Meeting; 2016 Apr 1-3; Boston, MA
The association between picoAMH levels and new-onset sleep disturbance in women during menopausal transition
Objective
To investigate 1) whether low concentrations of AMH predict the new-onset of sleep disturbance generally, and awakenings specifically, and 2) whether vasomotor symptoms (VMS) mediate an association between AMH and new-onset sleep disturbance or awakenings during the MT
Methods
1098 and 1166 participants in new-onset sleep disturbance and awakenings analyses, respectively were included in the study. Annual assessments of AMH levels, self-reported sleep disturbances and VMS were collected.
Results
519 (47%) women reported sleep disturbance and 493 (42%) reported awakenings during follow-up (mean 6.4 yrs). AMH was significantly negatively associated with new-onset of sleep disturbance (hazard ratio [HR] 0.90, 95% CI 0.82–0.998, p=0.047) and awakenings (HR 0.90, 95% CI 0.81–0.995, p=0.040) after adjusting for all covariates except VMS. VMS were significantly associated with AMH, new-onset of sleep disturbance and awakenings (all p<0.0001). After further adjustment for VMS, AMH was no longer associated with new-onset of sleep disturbance (HR 1.08, 95% CI 0.97–1.20, p=0.16) or awakenings (HR 1.07, 95% CI 0.96–1.09, p=0.25).
Conclusion
AMH predicts the development of sleep disturbance in general and awakenings, during the menopause transition, but this association is mediated by VMS, which appears to drive the association between declining AMH levels and new-onset sleep problems.
Reference:
Joffe H, Crawford S, Bromberger JT, Kalra B, Kumar A, Morrison A, Finkelstein J, Kravitz JM. Vasomotor Symptoms Mediate the Association Between Anti-Mullerian Hormone Levels and New-Onset Sleep Disturbance in Women during the Menopause Transition: Study of Women’s Health Across the Nation (SWAN). Presented at 98th Annual Endocrine Society Meeting; 2016 Apr 1-3; Boston, MA
Assessment of incidence of early natural menopause using MenoCheck (picoAMH)
Objective
To assess the risk of incident of early natural menopause in women aged 32–44 using picoAMH
Methods
Premenopausal blood samples were collected as part of prospective Nurses’ Health Study II cohort. Participants were followed for 12 years for early natural menopause. Early menopause cases (n = 327) were women reporting natural menopause between blood collection and age 45. Controls (n = 491) experienced menopause after age 45 and included 327 cases matched to controls on the basis of age at blood draw (±4 months).
Results
In multivariable conditional logistic regression models adjusting for matching factors, each 0.10 ng/ml decrease in AMH was associated with a 14% higher risk of early menopause (P < 0.001). The odds ratios for early menopause for women with AMH levels of 1.5, 1.0 and 0.5 ng/ml compared to 2.0 ng/ml were 2.6, 7.5 and 23 (all P < 0.001). Significant associations were observed irrespective of smoking status, adiposity, infertility history and menstrual cycle characteristics. Furthermore, models assessing the predictive ability of AMH showed high concordance, and C-statistics were high, ranging from 0.68 (age ≤35) to 0.93 (age 42).
Conclusion
This is the first prospective study to evaluate whether AMH levels are associated with early menopause. These findings support the utility of AMH as a clinical marker of early menopause in otherwise healthy women.
Reference:
Bertone-Johnson ER, Manson JE, Purdue-Smithe AC, Steiner AZ, Eliassen AH, Hankinson SE, Rosner BA, Whitcomb BW. Anti-Müllerian hormone levels and incidence of early natural menopause in a prospective study. Hum Reprod. 2018 Jun 1;33(6):1175-1182.
Utility of MenoCheck (picoAMH) for predicting the time to the final menstrual period
Objective
To predict the likelihood that a woman would have her final menstrual period (FMP) within a specified duration of time based on her AMH levels.
Methods
Serum samples 3302 women aged 42 to 52 years were collected and picoAMH levels were measured.
Results
Women whose AMH values were 5-10 pg/mL had a 50% chance of having their FMP within 11 +/- 2 months and a 75% chance of having their FMP within 24 +/- 3 months. Adding age to the model sharpened predictions across all AMH categories.
Conclusions
When very low, (< 10 pg/mL) AMH can help predict a woman’s chance of having her FMP in the next year with reasonable precision. Women with AMH levels > 20 pg/mL are unlikely to become postmenopausal in the next 2 years. AMH appears to be a reliable marker of ovarian aging that can help predict the FMP and may allow clinically useful predictions of other changes linked to the MT.
Reference:
Finkelstein JS, Lee H, Burnett-Bowie SAM, Santoro N, Yu EW, Joffe H, Morrison A, Kumar A, Greendale GA, Gold E, Harlow S, Lasley BL, Derby C, Randolph JF, Matthews KA, Kravitz HM, McConnell DS, Brooks MM, Martin D, Darakananda K, Hirsch SC, Sluss PM. Utility of Anti-Mullerian Hormone (AMH) for Predicting the Time to the Final Menstrual Period: The Study of Women’s Health Across the Nation (SWAN). Presented at 98th Annual Endocrine Society Meeting; 2016 Apr 1-3; Boston, MA
PODCAST – JAMA Clinical Reviews
Menopause is inevitable for women. It symptoms are uncomfortable and distressing. For women to best cope with menopause, it is useful to firmly establish the onset so that appropriate counseling can follow. In this podcast, an expert in this field, Nanette Santoro, MD, from the University of Colorado, explains how to diagnose menopause.
Santoro, N. (Speaker). (2019, July 22). JAMA Clinical Reviews: Diagnosing the onset of menopause [Audio podcast]. Retrieved from https://jamanetwork.com
How to Order MenoCheck
The MenoCheck test is currently performed at ARUP Laboratories and can be ordered through your local hospital lab.